If the plague, cholera or typhus seem to belong to the past for many societies in the world - the big names of those who revolutionized the field of infectious diseases in the 19th century are now fronting their institutions: Pasteur in France, Koch in Germany for example - the big book of infectious diseases cannot yet be closed.
The Asian flu of 1957-1958 claimed more than a million victims in the world, and so did the Hong Kong flu between 1968 and 1970. The beginning of the 1980s will never be dissociated from the emergence of HIV / AIDS, which claimed between 25 and 35 million victims until this day. Cholera has kept flaring up in waves of varying intensity since the 1990s. It affects between 1.3 and 4 million people according to the World Health Organisation (WHO). Finally, around 50,000 cases of plague have been recorded since the 1990s. A particularity of this disease is that it can circulate unnoticed for years and suddenly reappear in the form of epidemic outbreaks (such as in the Surat region in India in 1994, seasonal outbreaks in Madagascar…).
After World War II, the golden age of victory over infectious diseases proved an illusion. It had been fueled by the hopes following scientific discoveries, technological progress and the benefits from hygienist practices of the end of the 19th century. Things have changed however with time: the resisting capacity of societies and their weaknesses are not exactly of the same nature. On one hand, the knowledge and tools used to fight the diseases are way more elaborate today than they were in 1900, which allowed unprecedented victories (smallpox for example was eradicated in 1980). On the other hand, a significant demographic growth in a more mobile and interconnected world, the acceleration of urbanisation, the emergence of antimicrobial resistance, the persistence of poverty, the destruction of biodiversity… are all risk factors in the (re)appearance of global infectious diseases.
Risk is a complex concept. It is difficult to apprehend. It comprises two dimensions, both difficult to evaluate: the probability of the feared event occuring and the severity of its consequences. In the case of COVID-19, the pandemic seems to have come as a surprise, because of its unexpected outbreak, because of the conditions for its rapid spread from the most central parts of the global economic space, and because of its dramatic consequences.
What are the elements which favoured this surprise effect? Was it the probability that a global pandemic might occur underestimated? Is it the severity of the health, social, economic and environmental consequences of such an event which was underestimated? Or both? Even though the information flow has never been so intense and fast, it is hard to understand why national and international political responses failed to assess the right level of risk associated with this pandemic outbreak. We suggest some elements to answer these questions, relying on both the characteristics of recent epidemics and the characteristics of COVID-19.
Understanding the epidemic risks of the past twenty years.
Following the Severe Acute Respiratory Syndrome (SARS) pandemic in 2003, six epidemics have triggered public health emergency of international concern (PHEIC) from the World Health Organisation: 1/ Influenza AH1N1 in 2009; 2/ Ebola hemorrhagic fever in 2014; 3/ the fever epidemic from the Zika virus in 2016; 4/ Ebola again in 2018; 5/ the resurgence of polio in 2019; and 6/ COVID-19 in 2020. Since 2005, PHEIC refers to an extraordinary event qualified as such because of the risk it represents to international health and to which a coordinated action is required from national States. The recent global public health emergencies were characterised by two features: the diversity and extent of spaces affected on the one hand, and the mortality attributed to them on the other.
For example, new polio cases have only been located so far in poor regions of the world undergoing geopolitical conflicts, whereas the Zika virus appeared in South America with a rapid spread to the whole intertropical zone. Similarly, the transmission of the SARS pandemic was contained but this virus demonstrated an ability to spread very rapidly to large urban spaces (Hanoi in Vietnam, Hong Kong, Singapore or Toronto in Canada). For the past twenty years, new or re-emerging pathogens have shown their ability to spread fast and globally.
The impact of such global health emergencies on general mortality may have seemed limited in time (less than ten weeks for influenza H1N1 for instance) and in terms of the age categories affected: with an increased severity for populations aged 50+ (H1N1 or SARS), in conjunction with risk factors such as heart and dietary conditions or not. The carriers (symptomatic or asymptomatic) exhibited similar profiles, and the consequences on global mortality remained limited, but the effects of handling patients were considerable for health systems locally and regionally (SARS, Ebola, Zika).
COVID-19: a rather quiet switch from epidemic to pandemic
The geographic spread and mortality attributable to COVID-19 leave no doubt as to the severity of this global crisis. But when exactly did the infectious episode of the pathogen, initially compared to the seasonal flu by some political and scientific actors, become a threatening global pandemic requiring half of humanity to lock down?
A study shows that the circulation of the virus in the Italian province of Lombardy started at least in the beginning of January 2020 (or a month before the first cases officially recorded), and that the first cases of a still unknown viral pneumopathy seem to have been recorded in November 2019 in China, the warnings about an epidemic risk happened much later in China, in Asia and then throughout the world. On 23rd January 2020, the WHO emergency committee upped their threat level, [declaring](https://www.who.int/news-room/detail/23-01-2020-statement-on-the-meeting-of-the-international-health-regulations-(2005)-emergency-committee-regarding-the-outbreak-of-novel-coronavirus-(2019-ncov): “there exists an interhuman transmission of the virus (…) Some infected cases in China were exported to the United States, to Thailand, to Japan and the Republic of Korea.”
Starting in Wuhan, the virus transmission happened quietly, infecting a large number of people, most of them remaining asymptomatic. The sporadic cases qualified as “imported” - because they were linked directly to the original centre of the epidemic - led to more and more cases of local contamination. This process was accelerated by asymptomatic forms of the disease whose silent spread was reinforced by a rather long incubation period (up to two weeks). Besides, the mortality of 2%, estimated at the beginning of the epidemic in China, was not considered high enough to raise the alarm (the mortality rate of SARS or MERS-COV were estimated to be respectively 9.8 and 34%). Many comparisons, sometimes unfortunate, with the seasonal flu, introduced a confusion and underestimation of the risk.
Transmission routes have followed the channels of a globalised world. Wuhan, with over 11 million inhabitants, is the most populated city of Central China and the capital city of the Hubei province. It is an industrial, commercial financial and scientific centre. It is linked to the largest Chinese metropolises (Beijing, Shanghai, Guangzhou), all located within a 1000 kilometer range. Imported by airways, the epidemic then spread to different countries. From these first imported cases, local and community chains of transmission emerged. The characteristics of the first communities to be affected reflect their role in the globalised economy. In early February, Singapore had the highest number of infections outside of China and was planning to take restrictive measures as its financial centre was impacted; then Northern Italy, cradle of the “Made in Italy” luxury brands, became a new epidemic centre. Most cities in the world, being interconnected with China but also with each other, became affected by this epidemic because the symptomatic and asymptomatic characteristics of the disease made it hard to detect.
The possible organisational dysfunction in the relay of information about COVID-19
The identification of a new pathogen by the World Health Organisation relies on the national State’s sharing of information and on the representative WHO bureaus, which are not present in every country. Delays in information transmission from some of the States to the WHO may exist for several reasons: a will to downplay the severity or danger of the epidemic to preserve economic activities or political stability; a weakness of the health system and its ability to notify and register new risks and new diseases; some lags between the identification of the disease and the sharing of this information between difference administrative levels of a country, then to the WHO; the fact that a country might no be represented at WHO.
The ability of health systems to identify and to respond to epidemics is a crucial factor in case of emergencies. Over the past thirty or so years in most countries, healthcare systems have been profoundly transformed along two lines: a financial logic coupled with the contractualisation of means and objectives, and a multiplication of actors in charge of health. These changes may have pushed health systems to reorganise or reduce some programs, in particular those dealing with risk prevention, but also to extend the chain of actors in charge of health, making responses more complicated in case of health emergencies. Such dysfunction in the face of critical situations question the way States are organised.
For instance, in France - a country whose healthcare sector is still centralised, as is Spain despite an older dynamic of decentralisation - criticisms against national health structures have been sparked by the lack of anticipation regarding both prevention and the protection of people, healthcare workers and carers. In a federal system such as the United States, lockdown measures taken by some State governors have been criticized by Federal power. In Germany, where the Länder (or “regions”) cater for healthcare, the federal system was praised for its ability to offer tailor made responses to differentiated challenges, but it was also criticized for the delays imposed by coordination and competition on decision making and information transfer between administrative levels in times of crisis.
COVID-19: an epidemic so far removed…
Quite obviously, for a large number of rulers in the world, the risk of an epidemic seemed far removed at first. The first sources noting the novelty and danger of COVID-19 were sporadic, hard to trace and to evaluate because they were transmitted on Chinese social media, where information is tightly controlled by the central political power. Initially shared within scientific communities (through journals, blogs, etc.), the information was then relayed by national political actors while new sources of information appeared, through more official channels and at varying rhythms, seemingly at odds or quite late compared to the health situation.
In the end, it took the WHO about two and a half months to declare the situation as a pandemic, after a large number of countries were already affected. As a comparison, it took less than a month during the H1N1 epidemic between the identification of the first cases in Mexico on 5th May 2009 and the pandemic declaration on 2nd June 2009.
The initial resources produced by national governments were confusing because the different messages shared at the international level did not provide national level decision makers with real answers, but also because other political events closer to home delayed action on this information, such as pensions reforms and municipal elections in France, inter-community riots in India, etc.
Such ignorance of the actual risk level continued even during the first contaminations in each country. Information from China, Northern Italy or the first epidemic centres in each country could support the impression that the disease was spatially contained and only affected particular groups of people. It took the national lockdown measures for the whole population to regard the epidemic as immediate and dangerous. The change is illustrated by Google searches of the term “coronavirus between the 31/12/2019 (when the WHO received the first notification about the pneumopathy) and mid-April 2020 in four countries who chose to opt for strict or very strict national lockdowns.
Each country has its own epidemic curve, and similarly its own curve of relative interest in the term on the most popular search engine. We can see that “coronavirus” searches only become popular at the end of February 2020, so two months after the official declaration in China. Furthermore, WHO announcements and decisions about the risk level associated with COVID-19 seem to have had very little impact on the web searches. The epidemic remained far removed despite WHO alarms and announcements. However, the search peaks coincide with the chronology of lockdown announcements in all four countries: first Italy (step by step), then Spain, then France, then the UK.
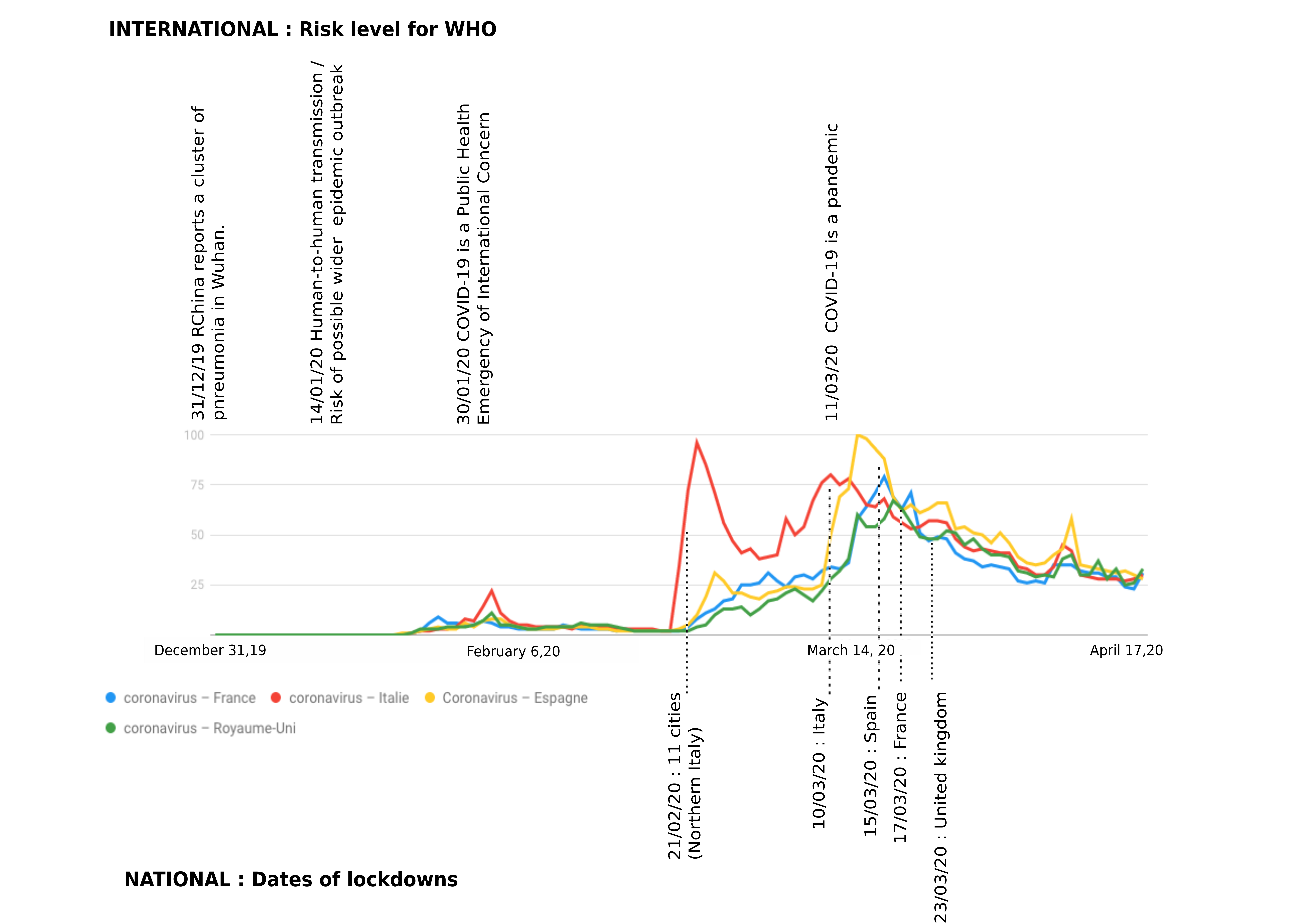
Chronology (31/12/2019-12/04/2020) of the search for “coronavirus” on Google in four european countries. “Google trends” gives the number of keyword searches as a ratio of the total searches made on Google at the given time. It highlights a particular interest for a given subject. Values represent the level of this interest by country and by day: 100 at the peak of term popularity, 50 when the term is half as popular and 0 when the number of searches is not high enough compared to other searches to represent a trend.
Conclusion
The “once in a century pandemic” announced in 2009 after the emergence of the A-H1N1 influenza virus generated a general and early mobilisation of national and international healthcare systems, whereas it seems that COVID-19, which we now know is more dangerous, has suffered from a combination of epidemiological and sociopolitical factors which made it more of a surprise epidemic.
The risk of an infectious disease with a potential to spread across the world was foreseen, but the international and national structures supposed to respond to it were not equally prepared. Scientific reports on global risks had not waited until 2020 to agree on the complexity and interdependence between multiple risks threatening the world equilibrium, a pandemic being one of the least negligible risks foreseen. The probability of such an event occurring is hard to estimate, but the potential severity of its consequences was already known as a hard fact. 2018, the unfortunate 100th anniversary of the “Spanish” flu, was an opportunity for scientists to recall that many epidemiological risks threaten our societies, and that they are never far away - in time or in space. During a conference titled “Are we ready for the next pandemic?”, Peter Piot, professor of public health and then director of the London School of Hygiene & Tropical Medicine was clear: our societies were insufficiently prepared for the new threats associated with infectious diseases. He offered several routes for improvement:
- Local capacities for detection and fast reaction should be reinforced within countries;
- Global health governance, represented by the WHO, should be strengthened;
- Partnerships and communication between communities, NGOs and the private sector should be more systematic;
- Data and sample sharing between scientific organisation and public healthcare systems should be automatic in due time;
- The Research & Development system should function independently from market incentives.
These five points were already part of the essential reforms sketched after Ebola in 2015. Even though Ebola did not manage to transform the rules enough to help with the current epidemic, will COVID-19 transform governance and practices in both national and international healthcare systems?